COVID-19 made a rapid, deadly march through the 106-bed Meridian Rehabilitation and Health Care Center, claiming nine lives and infecting 78 people in a matter of weeks.
The long-term care facility at 1555 N. Meridian, which has a history of health inspection problems, was identified last month as Sedgwick County’s second-deadliest COVID-19 cluster.
Only Clearwater Nursing and Rehabilitation Center has lost more residents — 12 — to the pandemic.
COVID-19 progressed quickly at Meridian, according to a timeline provided by the county. On Sept. 1, a county press release identified it as one of four long-term care facilities experiencing new clusters. Twelve Meridian residents and six staff members had been infected, but no one had died at that time, the press release said. By Oct. 8, nine residents had died, and by Oct. 16, 78 people had been infected there, according to the county. The cluster remained “open” or ongoing. A cluster is defined as two or more cases occurring at the same time and place. A cluster is considered closed when no new cases have been confirmed for 28 days.
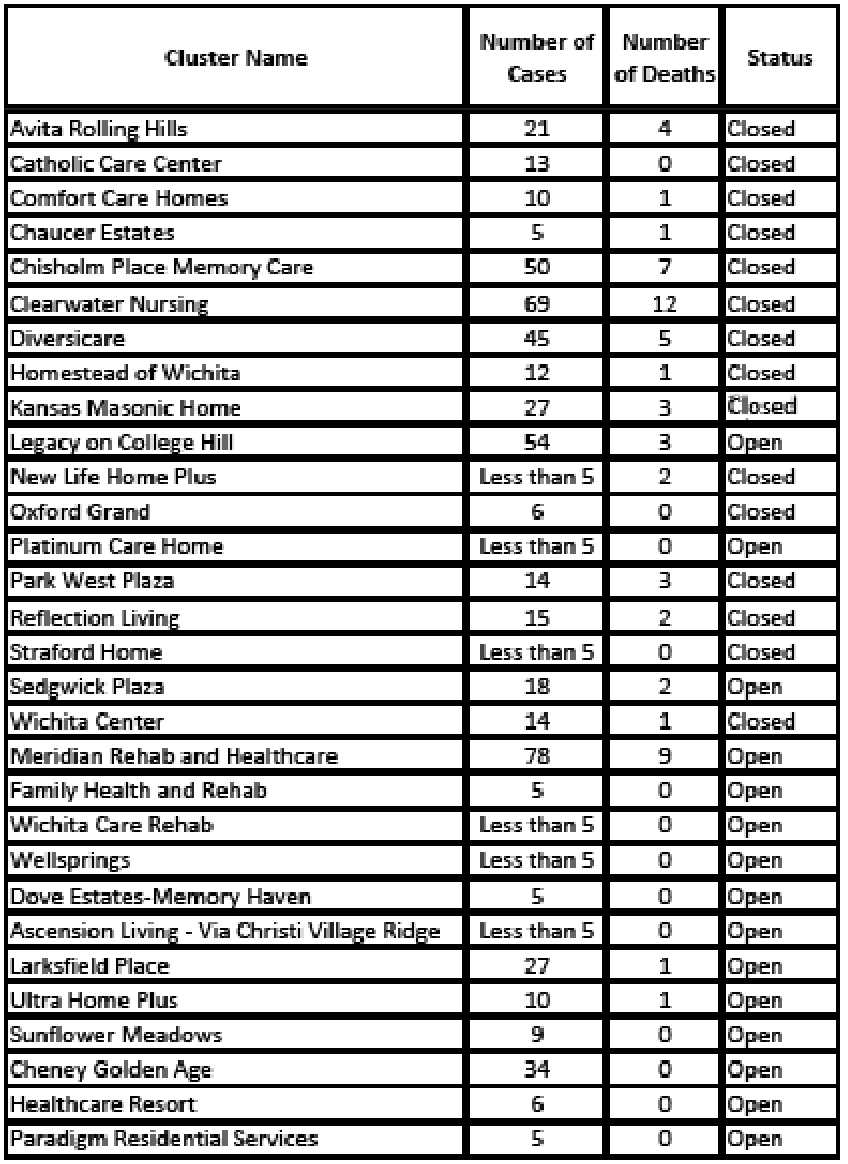
On Oct. 16, the county released a list of 34 clusters that have taken place here(See Chart Below). Seventeen remained open, including the largest, the Sedgwick County Detention Center, which has experienced 900 cases. Nursing homes and other long-term care facilities accounted for 30 of the clusters and 58 of the county’s 120 deaths through that date. Sixteen clusters in long-term care facilities remained open.
The administrator at Meridian referred questions to the corporate office in Kansas City, Mo. Tutera Investments LLC is the principal owner of the corporation behind the Wichita nursing facility. The Tutera Group, which has a multistate portfolio of senior living and health care facilities, did not respond to requests for comment this week. Tutera Group has facilities in northeast Kansas, but Meridian is its only care home in Sedgwick County, according to its website.
Meridian has 106 certified beds and accepts Medicare and Medicaid recipients. Past government inspections at Meridian have found deficiencies. On medicare.gov, where five stars is the best, Meridian’s current overall rating is one star. The federal government levied a fine of $32,760 in June 2019 and a fine of $7,150 in December 2017.
A standard health inspection was carried out in 2019, along with several complaint inspections. The total number of health deficiencies amounted to 33, compared to an average number of health deficiencies of 7.3 in Kansas facilities, and 8.3 nationwide, according to the Medicare website.
The 2019 inspection and complaint reports describe a facility short on fully trained staff, from nursing to the kitchen.
In January 2019, staff gave a resident eight times the correct dosage of medicine. A nurse did not call the practitioner to clarify the dosage because the practitioner had been rude and yelled during a previous phone call, the inspector was told. Staff later called the EMS to take the resident, experiencing a rapid, irregular heartbeat, to the hospital. The hospital contacted the Poison Control Center.
In May 2019, Meridian staff administered insulin to the wrong resident. In one case related to dietary services, a resident lost 18 pounds in six months. In another case, staff failed to provide the necessary services to keep a resident on supplemental oxygen before the tank ran out of oxygen.
A June 2019 inspection found Meridian’s infection control policy was last revised in August 2011.
Ronald Edward Bailey was a Meridian resident until late summer, when he went to Ascension Via Christi St. Francis with complications from an infection and then was transferred to a nursing home in Garden City. He died Sept. 6 at the age of 75. COVID-19 was not the cause of death.
His daughter, Ronda Bailey, was dismayed by the treatment he received at Meridian. She did not think staff dressed an infected wound properly or bathed him regularly. She said staff couldn’t tell her how long he was on the floor after a fall, and she said he was eager for her to bring him food.
“‘I need you now more than ever. Get me out of here,’” she said he told her.
After he was taken by EMS to the hospital, Bailey said, a hospital social worker called her regarding the condition of the infected wound and the care he had received prior to arriving at the hospital, she said.
“When he left St. Francis, they transferred him to Garden City, because we were not putting him back into Meridian,” Bailey said.
Coronavirus’ arrival in the U.S. prompted the Centers for Medicare and Medicaid Services in early March to order focused infection control surveys of federally certified nursing facilities, such as Meridian. On April 20, surveyors visited Meridian and found deficiencies.
Staff failed to follow the recommended 10-minute wait between applying a disinfectant on a hard surface and wiping the surface. One staff member said it was acceptable to spray it on and wipe it right back on; others said they let it set anywhere from one to five minutes. A housekeeping supervisor said it only had to be on the surface for a few seconds, according to the report available on the Kansas Department for Aging and Disability Services’ website.
Proper protocols for screening outside visitors to Meridian were not consistently followed, with staff failing to record the temperature of two visitors as required, the survey also said.
A follow-up survey found that Meridian’s deficiencies cited April 20 had been corrected and no new non-compliance was discovered.
The 78 cases at Meridian were the highest among local long-term care facilities, followed by 69 at Clearwater. The Clearwater cluster has been declared closed.
Deaths at long-term care facilities that have become COVID-19 clusters have contributed largely to the death toll across Kansas. As of Oct. 16, the Kansas Department of Health and Environment showed 405 of the state’s total 859 deaths from COVID-19 were linked to a long-term care facility cluster.
As of Oct. 7, Harvey County reported a total of eight deaths, including one resident of a long-term care facility. Harvey County Health Department Director Lynnette Redington declined to name that facility. It did have a cluster/outbreak associated with it at the time of the death, she wrote in an email.
Butler County Health Department Administrator Jamie Downs reported on Oct. 7 that there had been no deaths in long-term care facilities in Butler County. The county’s overall fatalities from the virus stood at three.
The breakdown of deaths at Sedgwick County long-term care facility cluster locations, as of Oct. 16, were:
Avita Assisted Living and Memory Care at Rolling Hills 4; ComfortCare Homes 1; Chaucer Estates 1; Chisholm Place Memory Care 7; Clearwater Nursing and Rehabilitation Center 12; Diversicare 5; Homestead of Wichita 1; Kansas Masonic Home 3; Legacy on College Hill 3; Meridian Rehabilitation and Healthcare Center 9; New Life Home Plus 2; Park West Plaza 3; Reflection Living 2; Sedgwick Plaza 2; Wichita Center 1; Larksfield Place 1; Ultra Home Plus 1.
Ronda Bailey said she’s been unable to wrap up matters with Meridian, where her father’s belongings remain. “They don’t return phone calls.”
This story was produced as part of the Wichita Journalism Collaborative, a partnership of The Active Age and six other media organizations working together to bring timely and accurate news and information to Kansans.